
The Role of Neurotransmitters in Attention, Focus and Behavior
Key Points:
- Approximately 6.76% of adults experience focus and attention related challenges.
- Neurotransmitters such as dopamine, norepinephrine, serotonin and acetylcholine play crucial roles in managing focus-related tasks.
- A balanced diet, regular exercise, and supplements can support neurotransmitter production and function. Consider food or supplements high in omega-3 fatty acids, vitamin D, magnesium and B vitamins for foundational support.‡
- Targeted supplements can support specific neurotransmitters that contribute to focus and attention: CogniPhos (acetylcholine), CurcumaSorb Mind (dopamine and serotonin) and DopaPlus (dopamine and norepinephrine).‡
Table of Contents:
- Introduction
- Key Neurotransmitters Involved in Focus
- Natural Ways to Support Neurotransmitter Balance
- Conclusion
- Resources
Introduction
For many, maintaining focus is a daily struggle that affects productivity and overall well-being. The prevalence of focus and attention issues is approximately 6.76%, or around roughly 366.33 million, adults globally.
What causes these challenges with focus? One crucial factor is the brain’s neurotransmitters. Focus involves the ability to sustain attention on a particular task or goal, while ignoring distractions. It is essential for effective work, learning and daily functioning. Maintaining focus can be difficult for many people, leading to decreased productivity and increased stress. In this blog, we’ll explore how neurotransmitters impact our ability to focus, the role they play in managing focus-related tasks and provide some lifestyle solutions to support focus.
Key Neurotransmitters Involved in Focus
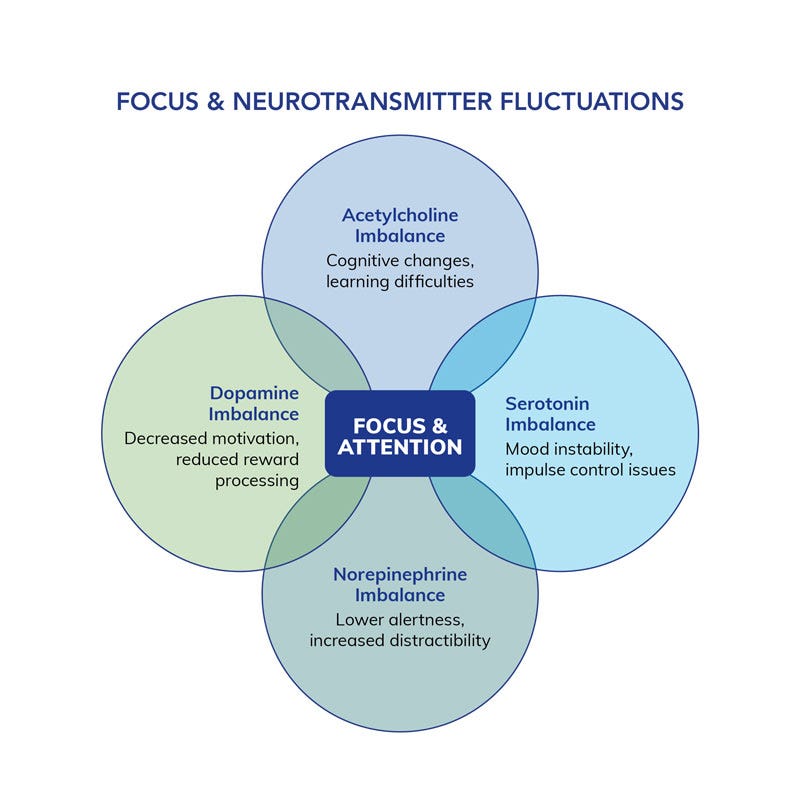
Dopamine: is essential for motivation, attention and reward processing. It helps regulate how we perceive and respond to stimuli, influencing our ability to stay focused on tasks. Low levels of dopamine can impair our ability to concentrate, stay organized, manage time effectively and may lead to challenges in maintaining attention on tasks.1
Norepinephrine: affects alertness and arousal. It helps the brain stay alert and responsive to stimuli, which is essential for maintaining focus. Norepinephrine has been shown to alter network activity in attention and working memory through arousal activation of the frontoparietal network, which is critical for sustained attention and alertness.2
Serotonin: influences mood, impulse control and overall cognitive function. It plays a role in managing emotional responses and maintaining a steady focus. Changes in serotonin levels can affect our emotional stability and our ability to maintain focus, leading to increased distractibility and impulsive actions.3
Acetylcholine: governs memory, learning, motivation and attention. Synthesized from choline, acetylcholine is the chief neurotransmitter of the parasympathetic nervous system and has a significant impact on muscle function, sleep, cognitive processes and mental performance.4 Fluctuations of acetylcholine can affect short-term memory, processing speed and word recall and can lead to learning difficulties and symptoms like brain fog.
Natural Ways to Support Neurotransmitter Balance‡
By understanding how neurotransmitters play a role in focus, attention and mood, you can better provide guidance on lifestyle changes that support neurotransmitter balance.
Diet and Nutrition
A balanced diet rich in essential nutrients can support neurotransmitter production and function. Foods high in omega-3 fatty acids and certain nutrients, such as vitamin D, magnesium and zinc, support the synthesis of neurotransmitters or assist their functioning.5
Very few research studies have investigated specific dietary patterns on focus or attention outcomes in randomized clinical trials. However, there is available evidence to provide broad recommendations, such as consuming nutrient-dense foods and limiting excessive added sugars as beneficial for attention problems.
Mediterranean diets, rich in omega-3s and plant-based foods compared to Western diets, have also been associated with better mental health and mood.6
Exercise
Regular physical activity has been shown to boost levels of dopamine, norepinephrine and serotonin, which can enhance mood and improve concentration. In fact, in children who have problems with attention, exercise interventions improved overall executive function when participating in exercise.7
Additionally, there is a robust body of scientific evidence demonstrating positive outcomes on brain function in adults from long-term exercise. Several studies have shown positive effects of exercise on cognitive functioning, specifically on prefrontal cortex-dependent cognition. Even acute, short bursts of exercise have been shown to improve mood and emotional status.8
Supplements
Various supplemental ingredients offer benefits to supporting neurotransmitter function.
- CogniPhos: A blend of clinically researched Cognizen® citicoline, acetyl-L-carnitine, Sharp-PS® phosphatidylserine and cofactors. Cognizen® promotes daily cognitive performance and mental sharpness. 9,10‡
- CurcumaSorb Mind: A curcumin and polyphenol blend to promote mood, memory and mental sharpness and support healthy levels of serotonin and dopamine. 11‡
- DopaPlus: This formula provides the dopamine precursors L-tyrosine and L-DOPA (from Mucuna pruriens). DopaPlus supports dopamine production and maintains healthy reuptake for daily mental function and sharpness. 12, 13‡
- Vitamin D + Magnesium: Vitamin D and Magnesium are both nutrients that play a role in the body’s nervous system. In a randomized-clinical trial, children supplemented with vitamin D and magnesium had a positive impact on and total difficulties compared to placebo after 8-weeks of supplementation.14‡
- Fish oils: are rich in omega-3 essential fatty acid. DHA, a fatty-acid in fish oil, is well recognized for its ability to support neural and cognitive function. Epidemiological studies indicate that intake of DHA is associated with healthy cognitive function.15‡
- Vitamin B6: A coenzyme involved in the synthesis of neurotransmitters needed for synaptic transmission (e.g., dopamine, serotonin, GABA).‡
- Pycnogenol®: A highly researched maritime pine bark extract, which contains a unique mixture of proanthocyanidins and other polyphenols. Clinical trials have shown that pycnogenol supports parameters related to attention in both children and adults. 17-19‡
Conclusion
Understanding the relationship between neurotransmitters and focus offers valuable insights into managing focus-related challenges. By addressing neurotransmitter imbalances through lifestyle changes and supporting supplements, individuals can help improve their ability to concentrate and enhance their overall focus and attention.
Resources
Mood Protocol: Developed in collaboration with our scientific and medical advisors to support mood.‡
Drug-Nutrient Interactions Checker: provides valuable information on potential interactions between your patients’ prescriptions, over-the-counter medications and nutritional supplements.
PureInsight™: Our streamlined platform easily collects patient data and provides valuable recommendations to help patients achieve their health goals.
Virtual Dispensary: Our Pure Patient Direct program provides account holders FREE access to our virtual dispensary to help simplify patient sales and reduce in-office inventory.
You can also explore Pure Encapsulations® to find On-Demand Learning, Clinical Protocols, and other resources developed with our medical and scientific advisors.
References
- Kessi M, Duan H, Xiong J, C, et al. Front Mol Neurosci. 2022 Sep 21;15:925049. doi: 10.3389/fnmol.2022.925049.
- O'Donnell J, Zeppenfeld D, McConnell E, et al. Neurochem Res. 2012 Nov;37(11):2496-512. doi: 10.1007/s11064-012-0818-x. Epub 2012 Jun 21.
- Jones LA, Sun EW, Martin AM, Keating DJ. Int J Biochem Cell Biol. 2020 Aug;125:105776. doi: 10.1016/j.biocel.2020.105776. Epub 2020 May 29.
- Sam C, Bordoni B. Physiology, Acetylcholine. [Updated 2023 Apr 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK557825/
- Lange KW, Lange KM, Nakamura Y, et al. Curr Nutr Rep. 2023 Sep;12(3):383-394. doi: 10.1007/s13668-023-00487-8. Epub 2023 Jul 28.
- Firth J, Gangwisch JE, Borisini A, et al. BMJ. 2020 Jun 29;369:m2382. doi: 10.1136/bmj.m2382.
- Liang X, Li R, Wong SHS, et al. Int J Behav Nutr Phys Act. 2021 May 22;18(1):68. doi: 10.1186/s12966-021-01135-6.
- Basso JC, Suzuki WA. Brain Plast. 2017 Mar 28;2(2):127-152. doi: 10.3233/BPL-160040.
- McGlade E, et al. J Atten Disord. 2015 Jul 15.
- McGlade E, et al. Food and Nutrition Sciences, 2012, 3, 769-773.
- Bhutani MK, et al. Pharmacol Biochem Behav.2009 Mar;92(1):39-43.
- Katzenschlager R, et al. J Neurol NeurosurgPsychiatry2004;75:1672-1677.
- Ranjbar E, et al. Nutr Neurosci.2014 Feb;17(2):65-71.
- Hemamy M, Pahlavani N, Amanollahi A,et al. BMC Pediatr. 2021 Apr 17;21(1):178. doi: 10.1186/s12887-021-02631-1. Erratum in: BMC Pediatr. 2021 May 12;21(1):230. doi: 10.1186/s12887-021-02683-3.
- Jackson PA, et. al. Br J Nutr.2012 Apr;107(8):1093-8.
- Calderón-Ospina CA, Nava-Mesa MO. CNS Neurosci Ther. 2020 Jan;26(1):5-13. doi: 10.1111/cns.13207. Epub 2019 Sep 6.
- Belcaro G, Luzzi R, Dugall M, et al. J Neurosurg Sci. 2014 Dec;58(4):239-48. Epub 2014 Mar 28.
- Luzzi R, Belcaro G, Zulli C, et al. Panminerva Med. 2011 Sep;53(3 Suppl 1):75-82.
- Trebatická J, Kopasová S, Hradecná Z, et al. Eur Child Adolesc Psychiatry. 2006 Sep;15(6):329-35. doi: 10.1007/s00787-006-0538-3. Epub 2006 May 13.


















